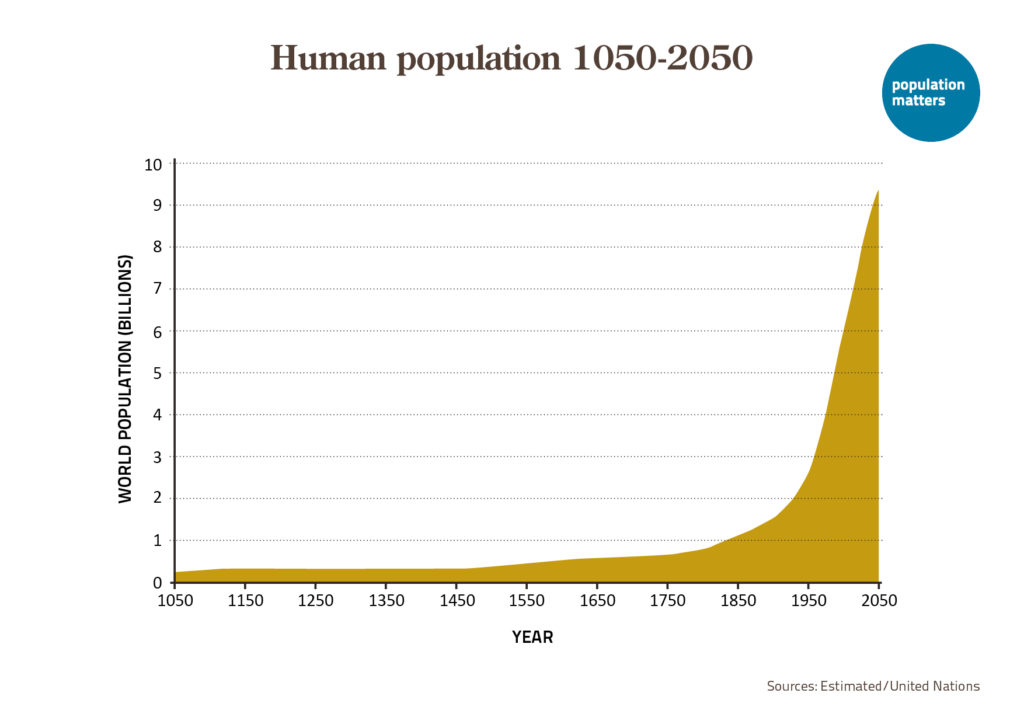
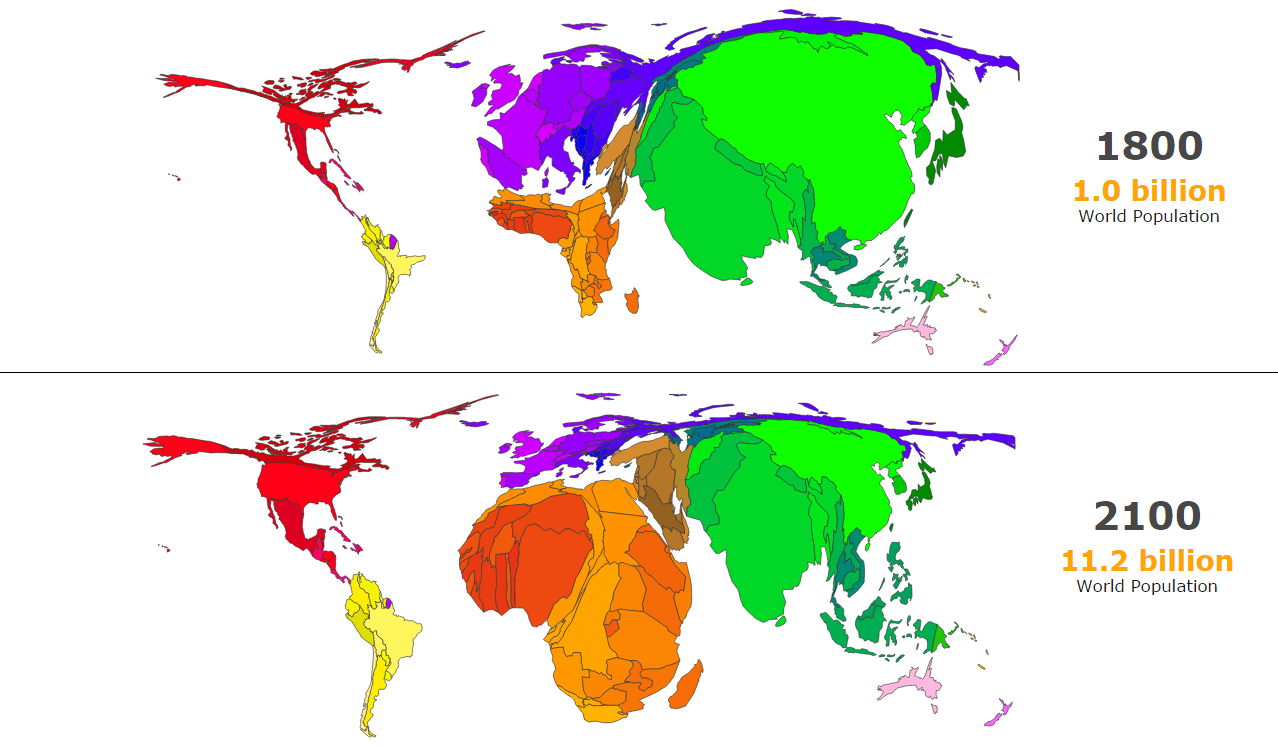
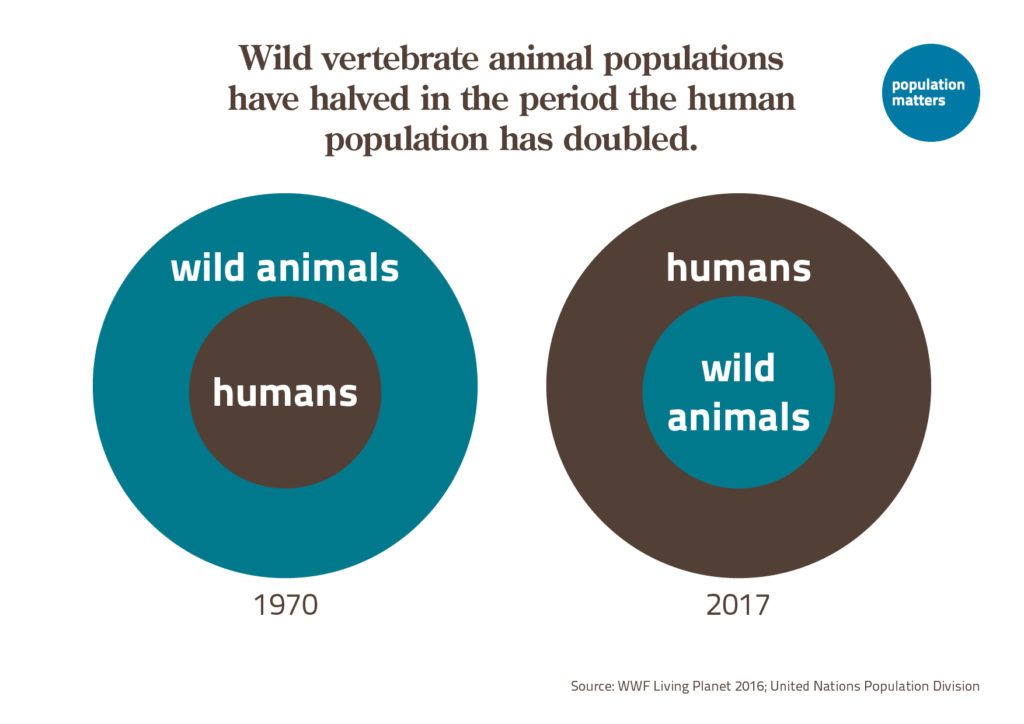
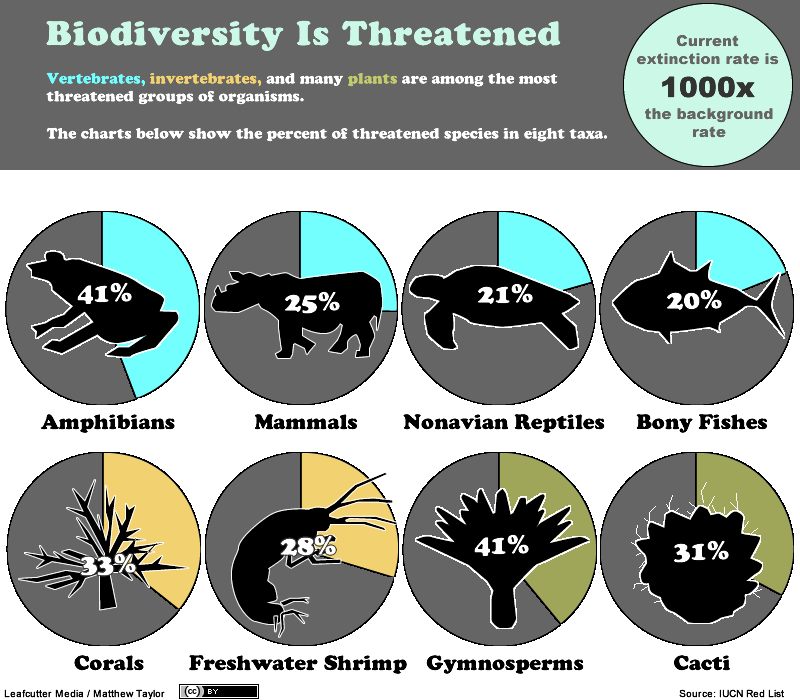
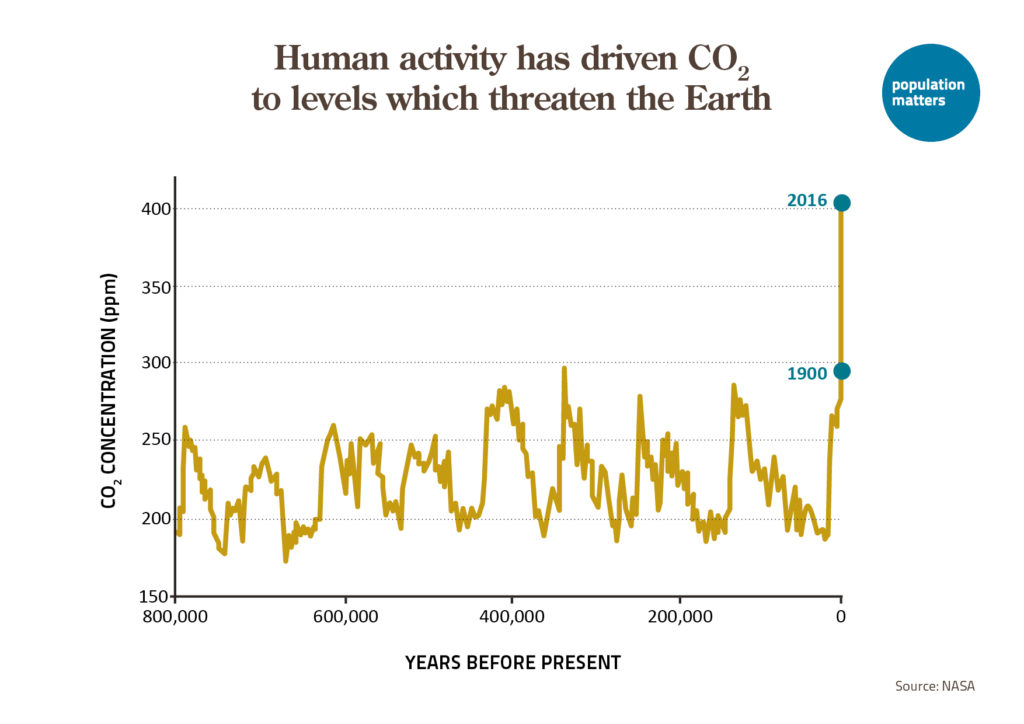
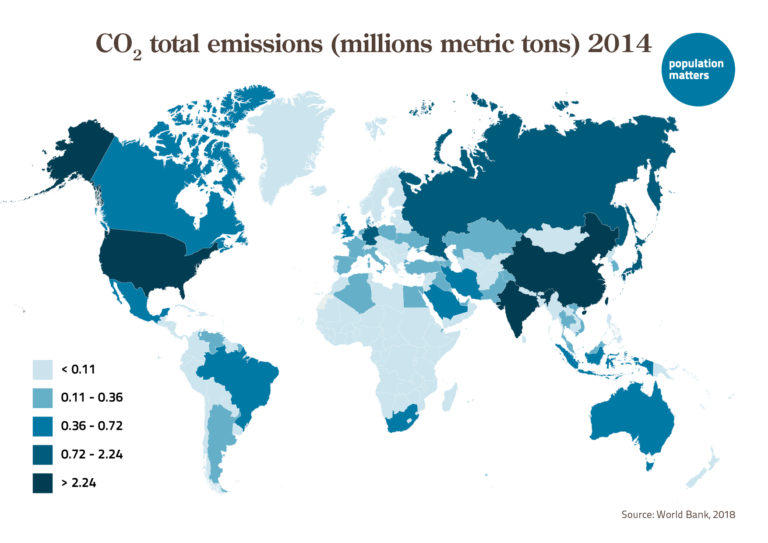
Over the past two centuries Earth’s human population has doubled, and doubled again, and doubled yet again, increasing from 1 billion to over 8 billion people. This huge increase is at the root of grave global environmental problems, from climate change to mass species extinction. The aim of The Overpopulation Project (TOP) is to study and highlight the environmental impacts of overpopulation, including humane policies to end population growth around the world. Initiated in 2017 with a generous two-year grant from the Global Challenges Foundation, TOP plans to continue its work through donations from supporters.

Our Motivation
People are overstressing the Earth: using too many resources, generating too much waste, and leaving polluted landscapes and empty seas in our wake. But this is the only home we have. Our descendants will depend on Earth’s ecosystem services for their health and well-being, just as we do. Ten million other species also need sufficient habitat and essential resources to survive and thrive. We have no right to extinguish them; instead, we have a responsibility to create ecologically sustainable societies that allow all Earth’s life forms to flourish.

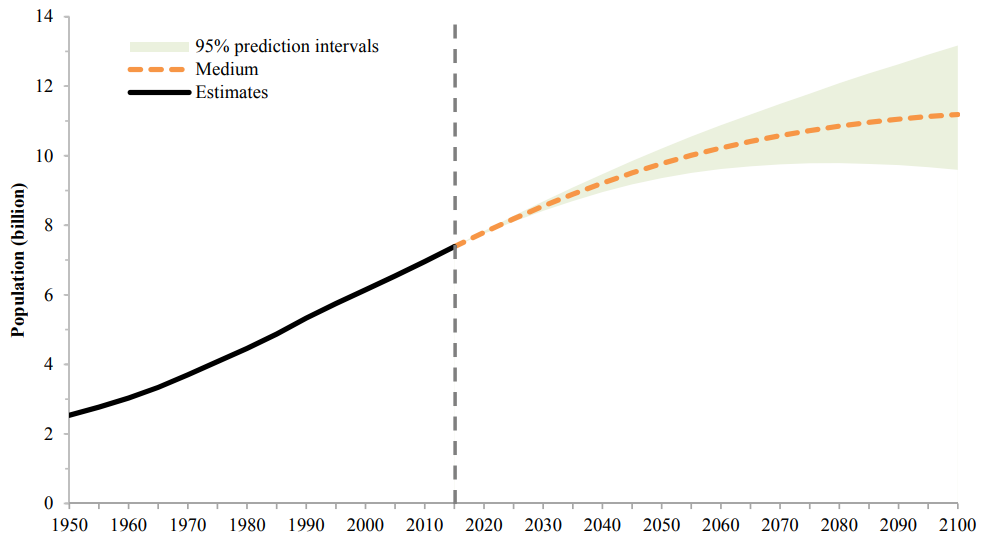
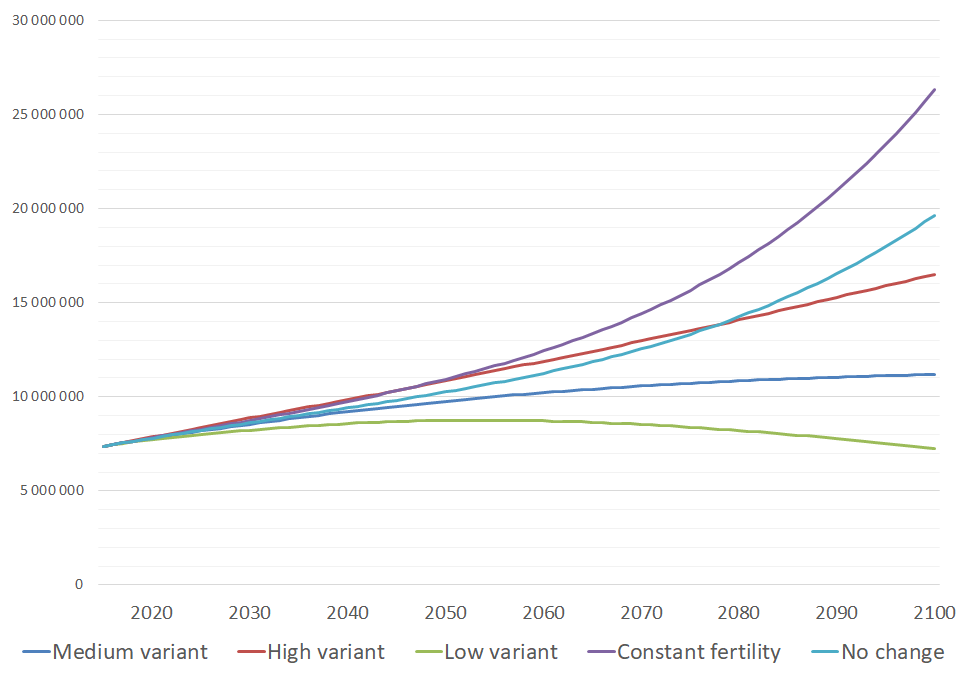
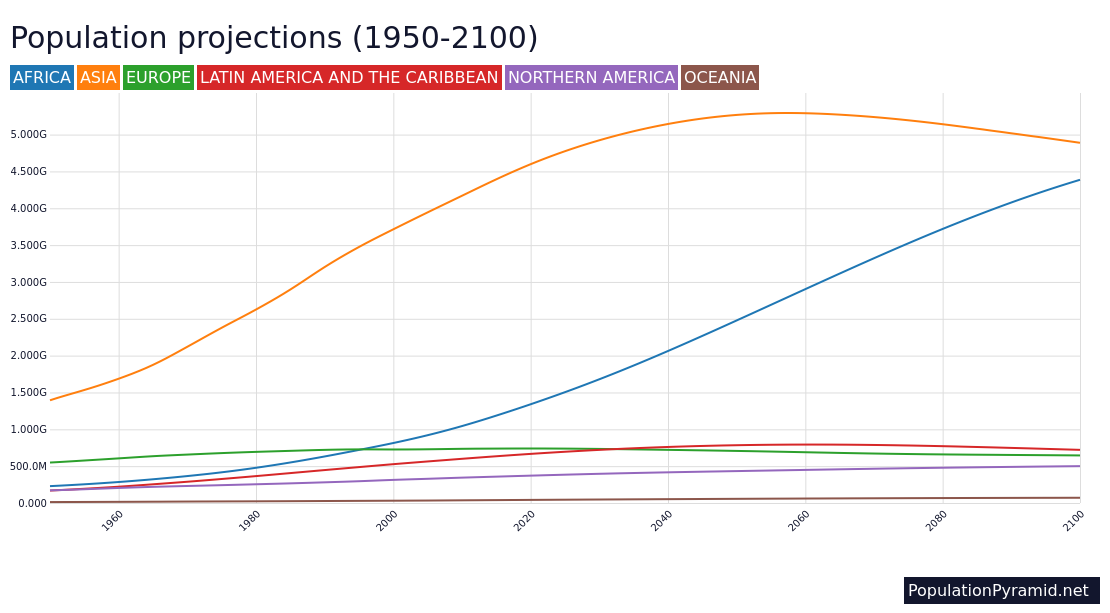
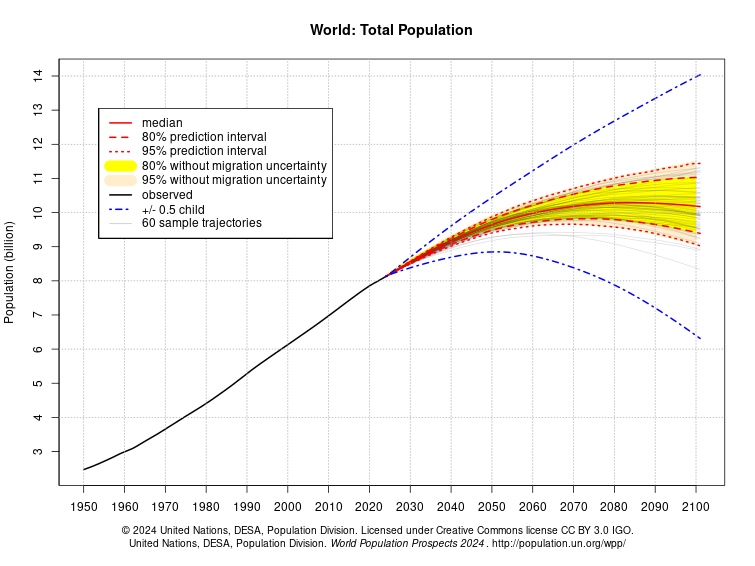
Limiting human numbers must be part of this effort. Yet environmentalists rarely acknowledge this—either because we think population growth is no longer a problem, or because we think the problem will solve itself. Neither is true. Excessive family size sends tens of millions of children to bed hungry each night in the developing world, where rapid population growth stresses scarce water, food and space resources beyond safe limits. Meanwhile continued population growth leads to deforestation, ailing coral reefs, and paved over farm lands and wetlands. Around the world, most national populations continue to grow and the United Nations projects a massive increase of 3 billion more people by 2100.
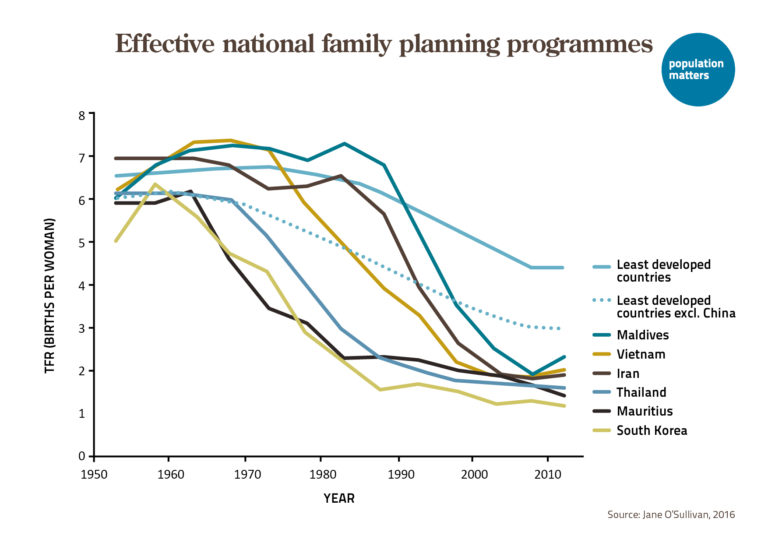
The Overpopulation Project studies the environmental impacts of overpopulation in an effort to remind environmentalists, scientists and policy makers of the contributions ending population growth can make in dealing successfully with global environmental problems. Believing that much of this century’s projected population increase could be avoided with the right public policies, it also explores humane policies to end population growth sooner rather than later.

The views and opinions expressed in guest blog posts are those of the authors and do not necessarily reflect the position of The Overpopulation Project.